Volume 33, Nº 3, May and June 2020
DOI: https://doi.org/10.36660/ijcs.20180021
ORIGINAL ARTICLE
Plasma Renin in Women Using and Not Using Combined Oral Contraceptive
Sidney de Souza Oliveira
Jefferson Petto, Diego Passos Diogo
Alan Carlos Nery dos Santos
Marvyn de Santana do Sacramento
Ana Marice Teixeira Ladeia
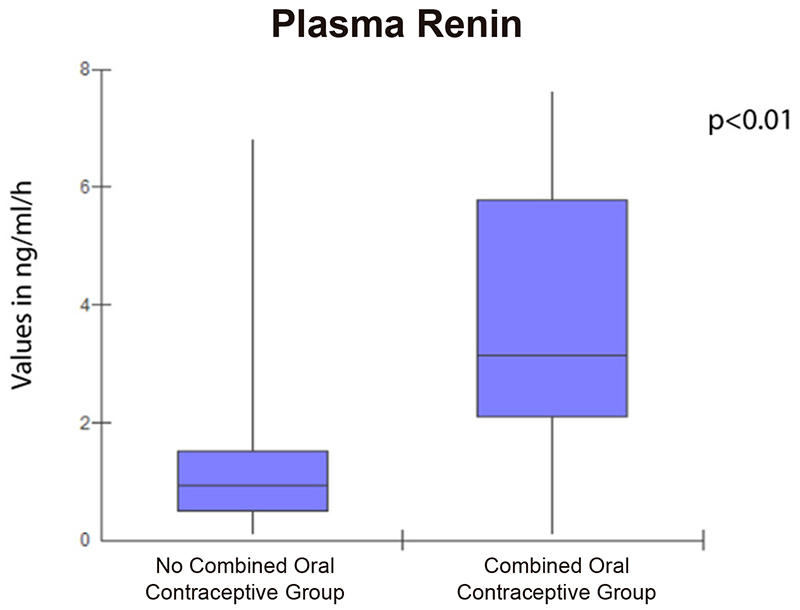
Figure 1 - Median and Interval quartiles of Plasma Renin from the studied groups.
Abstract
Background: Recent studies show that women on combined oral contraceptives (COC) present abnormal fasting lipid profile, increased postprandial lipemia, plasma C-reactive protein (CRP) and blood pressure (BP) compared to women not on combined oral contraceptives. Plasma renin is one of the factors responsible for abnormal BP.
Objectives: To assess plasma renin levels in women using or not using COC, the correlation between renin and CRP, as well as divergences in lipid profile.
Methods: A cross-sectional study with apparently healthy women aged 20 to 30, eutrophic, irregularly active, and with fasting triglycerides < 150 mg/dL. The sample was stratified into two groups: the No Combined Oral Contraceptive Group (NCOCG), comprised of women who did not use any type of hormone contraceptive, and the Combined Oral Contraceptive Group (COCG) comprised of women on low-dose COC for at least one year. After a 12-hour fast, 5 ml of blood was collected for renin dosing and PCR. Data were analyzed by the t-Test and bidirectional Mann-Whitney Test, both with significance < 0.05.
Results: We evaluated 44 women equally distributed between the groups, age 23 ± 1.2 years, BMI 21.0 ± 3.2 kg/m2. Median and interquartile deviation of renin in the NCOCG and the COCG were, respectively, 0.5 (0.1-1.0) and 3.0 (2-6) (p < 0.01). A positive correlation between PCR and renin (p < 0.01 and r = 0.68) was found.
Conclusion: The plasma renin levels of women using COC were higher, with a strong correlation with CRP. (Int J Cardiovasc Sci. 2020; 33(3):208-214)
Keywords: Hypertension; Metabolism; Contraceptive, Agents; Risk Factors; Genetics; Dyslipidemias; Diabetes Mellitus; Sedentarism, Women’s Health.











