Volume 112, Nº 1, January 2019
DOI: http://www.dx.doi.org/10.5935/abc.20180247
ORIGINAL ARTICLE
Rapamycin Combined with α-Cyanoacrylate Contributes to Inhibiting Intimal Hyperplasia in Rat Models
Tianshu-Chu
Congrong-Gao
Zhiwei-zhao
Fei-Ling
Ayu-Sun
Yuanbiao-Zheng
Jing-Cao
Jianjun Ge
Dr. Tianshu-Chu
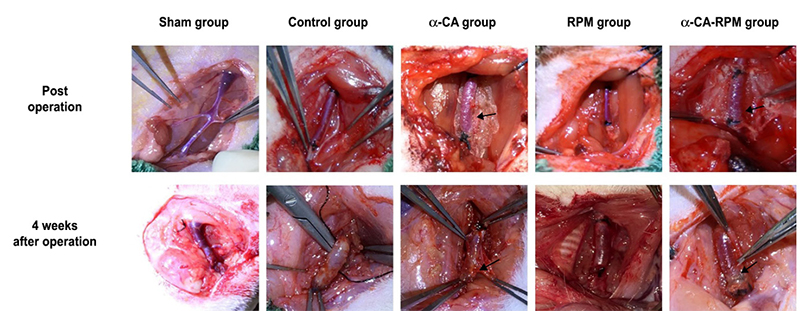
Figure 1 – Rats survived well 4 weeks after operation. Operating procedure as previously described was used to build models of grafted rat jugular vein on carotid artery on one side. Post-operation, the transplanted veins are well filled and the blood vessels beat well, and the glue was spread evenly over the surface of the veins in the α-CA and α-CA-RPM groups (arrow). Four weeks after operation, veins in the sham group slightly expanded; the control group had new granulation tissue, thickening tubes, edema and light stiffness; the α-CA group had few fresh tissues which were easily separated, with no obvious expansion and clear boundary from the surrounding, and the glue was not fully degraded (arrow); the RPM group had clear boundaries from the surrounding tissue, and they were fresh and no obvious expansion. The general form of α-CA-RPM group was similar to α-CA group.
Abstract
Background: Vein graft restenosis has an adverse impact on bridge vessel circulation and patient prognosis after coronary artery bypass grafting.
Objectives: We used the extravascular supporter α-cyanoacrylate (α-CA), the local application rapamycin/sirolimus (RPM), and a combination of the two (α-CA-RPM) in rat models of autogenous vein graft to stimulate vein graft change. The aim of our study was to observe the effect of α-CA, RPM, and α-CA-RPM on vein hyperplasia.
Methods: Fifty healthy Sprague Dawley (SD) rats were randomized into the following 5 groups: sham, control, α-CA, RPM, and α-CA-RPM. Operating procedure as subsequently described was used to build models of grafted rat jugular vein on carotid artery on one side. The level of endothelin-1 (ET-1) was determined by enzyme-linked immunosorbent assay (ELISA). Grafted veins were observed via naked eye 4 weeks later; fresh veins were observed via microscope and image-processing software in hematoxylin-eosin (HE) staining and immunohistochemistry after having been fixed and stored” (i.e. First they were fixed and stored, and second they were observed); α-Smooth Muscle Actin (αSMA) and von Willebrand factor (vWF) were measured with reverse transcription-polymerase chain reaction (RT-PCR). Comparisons were made with single‑factor analysis of variance and Fisher’s least significant difference test, with p < 0.05 considered significant.
Results: We found that intimal thickness of the α-CA, RPM, and α-CA-RPM groups was lower than that of the control group (p < 0.01), and the thickness of the α-CA-RPM group was notably lower than that of the α-CA and RPM groups (p < 0.05).
Conclusion: RPM combined with α-CA contributes to inhibiting intimal hyperplasia in rat models and is more effective for vascular patency than individual use of either α-CA or RPM. (Arq Bras Cardiol. 2019; 112(1):3-10)
Keywords: Myocardial Revascularization/surgery; Cyanocrylates; Sirolimus; Hyperplasia; Graft Occlusion, Vascular; Vascular Patency; Rats















